Using Hiring Data to Improve Workforce Planning
Mar 30, 2026

US healthcare leaders battle persistent staffing gaps—over 120,000 nursing positions remain unfilled in 2026 amid rising patient loads from chronic diseases and seasonal surges. Manual gut-feel planning fails here, leading to overtime spikes costing $7 billion yearly and delayed care in overwhelmed ERs. Hiring data changes the game, transforming reactive firefighting into predictive workforce strategies that align talent with demand.
Analytics platforms crunch historical hires, turnover patterns, and external trends like CDC flu forecasts, enabling hospitals to staff proactively for peaks in states like Texas or New York.
Why Data Beats Intuition in Healthcare Staffing
Traditional planning relies on spreadsheets and hunches, missing nuances like 20% seasonal turnover in Florida clinics or ICU nurse shortages during winter RSV waves. Without data, 60% of US health systems overstaff off-peaks or understaff crises, per industry benchmarks.
Data illuminates blind spots:
Historical fill rates reveal bottlenecks—e.g., 45-day delays for surgical techs.
Turnover analytics flag high-churn roles like telemetry nurses (25% annual rate).
External signals like aging demographics predict 15% demand growth by 2030.
Hospitals ignoring this face CMS penalties for ratio violations (1:4 in California ICUs) and agency fees hitting $90/hour.
Key Metrics to Track for Smarter Planning
Focus on actionable hiring data tailored to US healthcare:
Time-to-Fill: Target under 14 days for temps; track by role and region.
Cost-per-Hire: Benchmark $4,000 for RNs, factoring agency premiums.
Quality-of-Hire: Measure 90-day retention and patient satisfaction scores.
Demand Forecasting: Blend EHR volume data with CDC trends for surge predictions.
Diversity Metrics: Monitor underrepresented hires to meet Joint Commission goals.
Dashboards aggregate these, spotting patterns like Midwest hospitals needing 30% more CNAs during harvest-related injuries.
Building a Data-Driven Workforce Planning Framework
Step one: Centralize data from ATS, HRIS, and payroll into one platform. AI models then forecast needs—e.g., predicting 25% ER volume jumps from flu data.
Implementation pillars:
Predictive Modeling: Simulate peaks using 3-year hire history plus real-time census.
Scenario Planning: Test "what-if" for nurse strikes or elective surgery backlogs.
Gig Pool Analytics: Track verified temp availability for on-demand scaling.
Compliance Integration: Flag license expirations pre-peak to avoid fines.
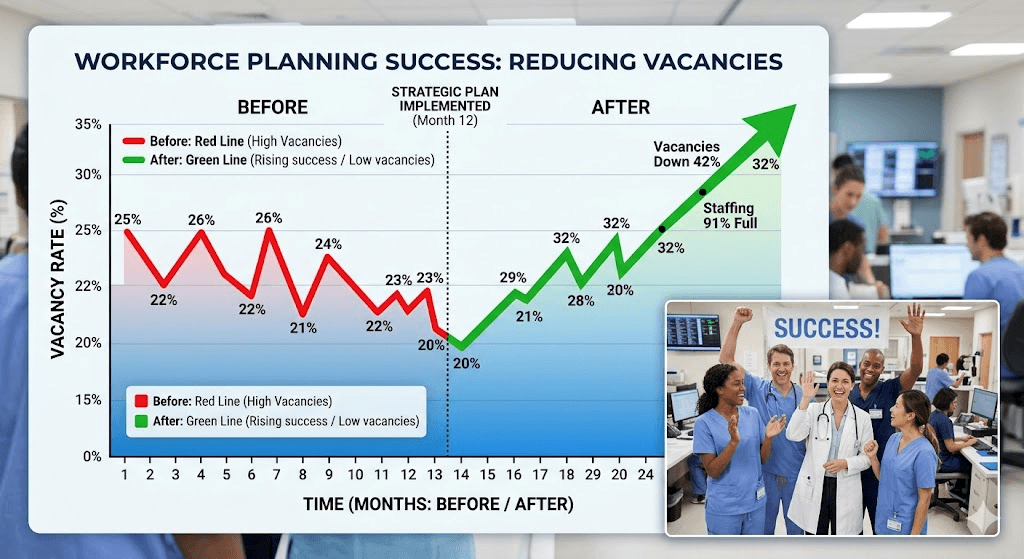
A 2026 health system survey showed data users cutting vacancies 40% while trimming fixed costs 25% via flexible gigs.
Case Studies: Data Wins in US Healthcare
A Chicago network analyzed 2025 hiring data, spotting oncology nurse gaps during chemo surges. Predictive tools built a pre-vetted pool of 200, filling 95% of shifts internally versus 70% agency-dependent before—saving $2M annually.
In Arizona, data revealed seasonal travel nurse preferences, optimizing incentives to boost local retention 30%. Another Texas system used turnover heatmaps to target high-risk units, reducing churn 22% through proactive re-skilling.
Overcoming Data Silos and Skill Gaps
Legacy systems fragment info—EHRs don't talk to ATS. Solution: API-integrated platforms with no-code dashboards. Train non-tech staff via intuitive visuals; start with one department.
Privacy matters: HIPAA-compliant aggregation anonymizes data while flagging trends like sanction risks on OIG lists.
Master Workforce Planning with Gigin Health
Gigin Health empowers US healthcare with AI-driven hiring analytics: Forecast peaks, track metrics, and deploy verified gig talent seamlessly. From nurse pipelines to compliance dashboards, optimize every hire.
Sign up for a free demo at gigin.health today. Turn data into dominance—staff smarter, not harder.